What Can I do for a Frozen Shoulder?
There are times when shoulders simply freeze. The causes can be chalked up to something as mundane as staying in a position too long, or to more common health conditions like hypo and hyperthyroidism, diabetes, stroke, and cardiovascular disease.
Frozen shoulder, also known as adhesive capsulitis, is believed to be caused by an inflammatory response to the joint capsule (the ligaments that surround the shoulder joint) and the resulting adhesions and scar tissue, which prevent normal movement. The condition is very common in 40-60 year olds, with women more likely to suffer from a frozen shoulder.
What are the symptoms of frozen shoulder?
The hallmark symptom of frozen shoulder is persistent pain and limited range of motion. As time goes on, movement can become progressively limited with the shoulder becoming stiff, making it difficult to move the area without pain. Signs and symptoms typically develop gradually, sometimes over the period of months. There are three stages used to classify adhesive capsulitis:
Stage 1: Freezing
In this stage, pain increases gradually, making it harder to move your shoulder. As the pain worsens, there is loss of motion in the shoulder. The freezing stage lasts from 6 weeks to 9 months.
Stage 2: Frozen
Pain many decrease at this stage, but the stiffness remains. Normal daily activites may become difficult as the range of motion is strained. This stage lasts from four to six months.
Stage 3: Thawing
Shoulder motion gets easier, with range of motion slowly increasing over time. Pain may still be intermittent. This stage lasts between 6 months and 2 years.
What causes a frozen shoulder?
The capsule of connective tissue that surrounds the bones and ligaments of your shoulder joint can become thickened around the joint, restricing movement and stiffening the shoulder. The main risk factors are age, injury, and diseases like diabetes and cardiovascular disease. Some of the most common causes are:
Immobilzation
The risk of developing a frozen shoulder increases when recovering from surgery, injury, stroke or a procedure that prevents your arm from having full range of motion. While most sports related injuries result from over-use of a limb, frozen shoulder is a result of under-use injury, prompted by a period of restricted shoulder movement. Immobility may be the result of many factors, but the most common are:
- Rotator cuff injury
- Stroke
- Surgery recovery
- Bone spur
- Shoulder bursitis
- Osteoarthritis
Diabetes
More than 10 percent of the world’s adult population suffers from the diabetes. Because of the increase of this condition, frozen shoulders are becoming more of a frequent phenomenon, with over 12 percent of patients reporting frozen shoulder symptoms. There is a belief that long term high glucose levels in diabetics may change the connective tissues surrounding the shoulder.
Other Diseases
Medical problems that may increase the risk for frozen shoulder are:
- Hypothyroidisim
- Hyperthyroidism
- Cardiovascular disease
- Parkinson’s disease
What treatments are available for frozen shoulder?
When it comes to treating frozen shoulder, the goal is to control pain and restore full range of mobility and strength to the affected shoulder. Many patients have found relief through these promising treatments:
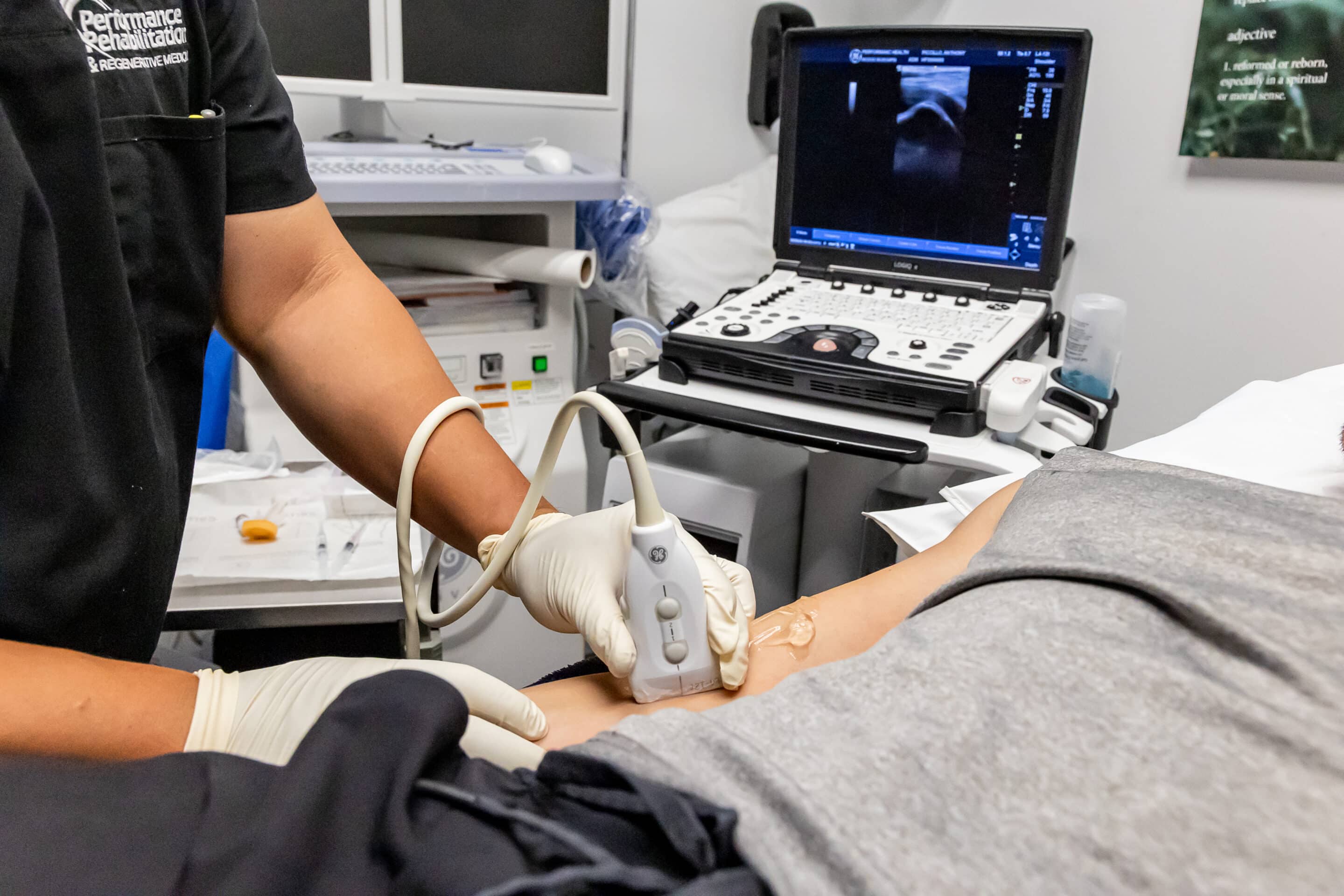
Physical Therapy
A physical therapist specializes in range of motion exercises to help restore mobility back to the affected shoulder. Patient cooperation and commitment is paramount to the success of this treatment.
Cortisone Injection with Joint Distention
An application of a powerful anti-inflammatory steroid called Cortisone is injected into the affected area, reducing inflammation and swelling of the surrounding nerves. Joint Distention involves an injection of sterile water into the joint capsule to expand the area, stretching the tissue and making it easier to move the joint.
Dry Needling Therapy
This therapy provides rapid healing to the connective tissues that are seizing up the shoulder. Dry Needling involves the insertion of a very fine, solid filament needle into a tight band of muscles and/or trigger point(s). The term “dry” needling means there are no medications (such as cortisone or lidocaine) injected into the muscle. Most patients report the insertion of the needle is painless.Most patients will notice measurable improvements within six treatments.
Active Release Technique
In ART, the treating physician/therapist will use their hands in a manual technique to identify regions of dysfunctional muscle, ligament or tendon tissue. Once identified, the physician/therapist will apply specifically directed pressure over the affected or related anatomical structures while the patient performs specific body movements. Most patients will notice an improvement over several sessions.
If your seeking relief from frozen shoulder, please feel free to contact one of our Patient Care Coordinators today at 908-754-1960 or book an appointment online.