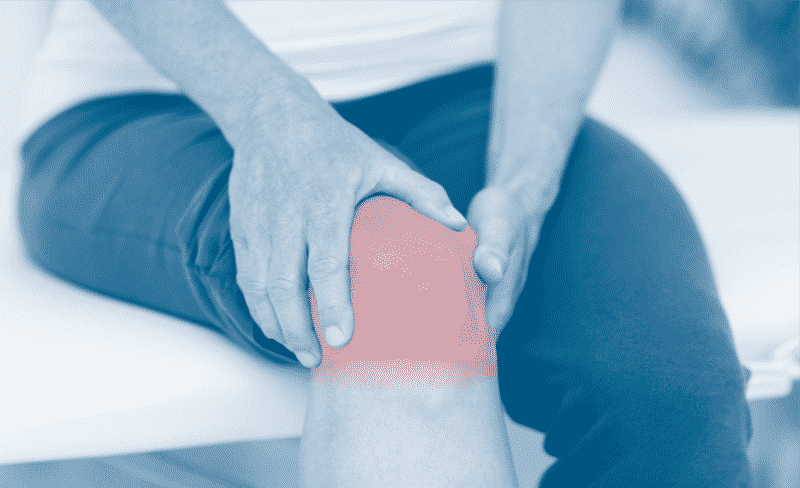
How Does Bone on Bone Knee Pain Feel?
Osteoarthritis is a degenerative joint disease that causes your joint tissues to degrade over time, setting off an inflammatory reaction that causes pressure placed directly on the bone of the knee. At first, symptoms are mild, but as the condition progresses, pain can become intense while performing daily activities, with quality of life markedly decreased due to limited mobility.
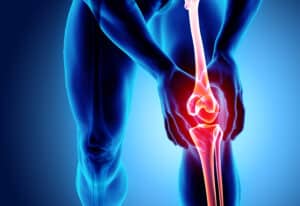
A healthy knee contains a soft spongy tissue between the bones called cartilage. This tissue acts as a natural shock absorber on either side of the knee. Synovium is the soft tissue that lines the joints. It produces a fluid called synovial fluid, which lubricates and supplies oxygen and nutrients to the cartilage.
Throughout the stages of osteoarthritis, the cartilage breaks down and wears away, making the bones under the cartilage rub together. When you experience bone on bone knee pain, generally the knees lack the synovial fluid needed to allow the joints to glide smoothly over each other, therefore a bone on bone knee pain injection is administered.
Typically, osteoarthritis is divided into four stages:
- Stage 1- Symptoms in this stage are mild, involving minor bone spur pain in the knee. This stage is usually remedied with over the counter (OTC) medications used to relieve discomfort and pain.
- Stage 2- At this stage, minor pain is experienced after walking or running, with joint stiffness and tenderness in the knee area. Knee cartilage remains a healthy size, and the bones are not rubbing or scraping against each other.
- Stage 3- During this moderate stage, the cartilage in the knee begins to narrow, causing discomfort during everyday activities. Pain may be more extreme after running, walking, kneeling or bending. After long periods of sitting, your knee may be stiff upon standing, and it may be difficult to bend or straighten the knee.
- Stage 4-The most severe stage of osteoarthritis, the cartilage in the knee has been significantly reduced or dissipated completely, leaving the joint stiff and likely immobile. The bone on bone pain causes great pain when moving the knee joint.
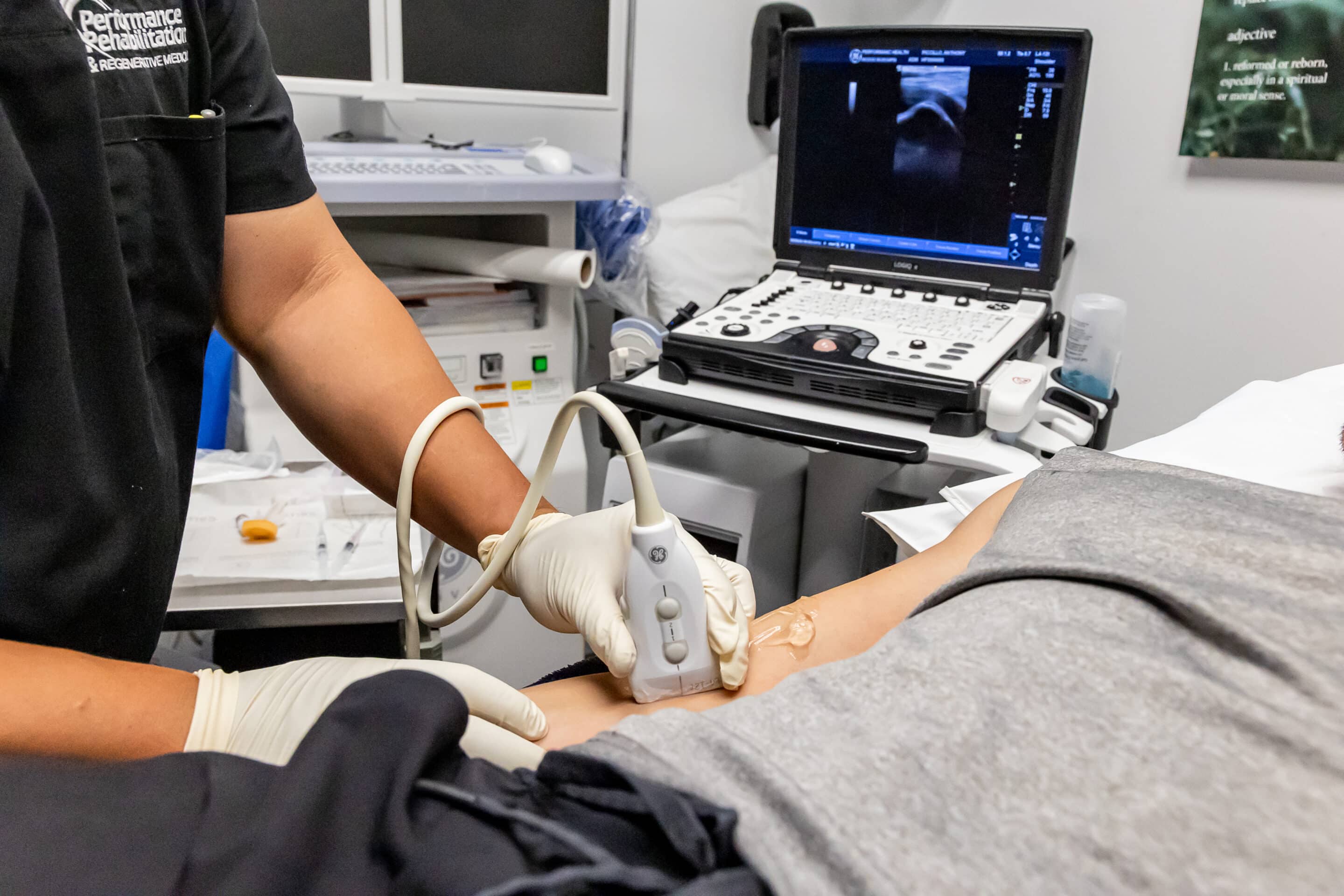
It is important to note that diagnostic imaging may appear to show bone on bone, but this is typically not the case. True bone on bone is very rare and often misdiagnosed. When it comes to treating acute or chronic knee pain, knee surgery tends to be a daunting prospect to patients. With many alternatives available, relief can be found without surgical intervention.
Weight loss
Carrying extra weight can cause additional stress on your joints, accelerating the onset of osteoarthritis and bone on bone knee pain. According to the Johns Hopkins Arthritis Center, for every extra ten pounds of weight you carry, there is an additional thirty to sixty pounds of force placed on your knees with each step.
Physical Therapy
Exercise and physical therapy is an integral part of dealing with the pain of osteoarthritis. At the outset of treatment, a highly trained physical therapist will perform a comprehensive evaluation. Their findings and treatment plans will be custom tailored to the patient’s individual needs in a shared decision-making model of patient care.
Hyaluronic Acid (HA) Injections
Hyaluronic acid is similar to a naturally occurring substance in the joint. It works by acting as a lubricant and shock absorber that helps the joint to work properly. A Joint Gel Injection can alleviate pressure, decrease pain, and increase range of motion. The HA treatments are an outpatient procedure typically conducted three to five times with a week in between.
Genicular Nerve Ablation
This innovative technology uses selective radio waves to block pain signals from the genicular nerves (nerves around the knee joint), to relieve knee pain and return you back to your daily activities. This in-office, non-surgical treatment takes 30 minutes and is performed under a local anesthetic. Genicular ablation is a safe, effective and minimally invasive procedure.
Prolotherapy
Prolotherapy is a procedure that involves injecting a non-pharmacological solution into dysfunctional tendons and ligaments with the intent of strengthening weak soft tissue structures that surround the joint, resulting in increased flexibility, stability, and endurance of the joint. The treatment is administered through a slender needle to the injured body part, administered in two to six week intervals. The entire procedure takes about 30 minutes and is performed in office under local anesthetic.
If you have any questions or you want to make an appointment please call one of our Patient Care Coordinators at 908-754-1960or you may book an appointment online.