Adult Stem Cell Therapy
Adult stem cells and their application for the treatment of orthopedic conditions has been gaining speed and growing evidence in recent years. Patients seeking a new alternative to traditional medicine have found lasting results with the implementation of their body’s own healing and the use of their own stem cells to promote that healing.
In recent medical history, a focus on healing the body through more natural means has come to the forefront. Where traditional medicine has fallen short and continues to look for answers, a new type of medicine has emerged, Regenerative Medicine. Using the body’s own healing properties to focus in on injured tissue, regenerative medicine continues to gain ground in health care.
Although broad by definition, regenerative medicine primarily involves two individual procedures, Adult Stem Cell Therapy and Platelet Rich Plasma Therapy (PRP). Both techniques focus on the concentration of a substance that targets injured or absent tissue. In orthopedics, these procedures have great promise for their uses on injuries to bone, cartilage and muscle tendon. These procedures have seen positive results in treatment of the shoulder, knee and other joints. For the purpose of this essay, adult stem cell therapy will be the main topic.
The rotator cuff is a group of four muscles that produces movement in the shoulder. The four muscles which include the supraspinatus, infraspinatus, teres minor and subscapularis, attach the scapula to the head of the humerus and provide movement and stability to the shoulder. The tendons form a capsule or a cuff around the shoulder joint providing structural support and functional movement.
Injury to the rotator cuff is a common condition of the shoulder that affects individuals from many backgrounds and activities. Injuries of these tendons are understood to impact 1 in 5 adults in their lifetime. Common injuries include: tears to the tendon, tendinitis and other tendinopathies.
A common condition within the knee found in athletes, both professional and weekend warrier, is injury to the anterior cruciate ligament (ACL). The ACL is a ligament that attaches to the tibia and femur. The placement and attachments of the ligament assist in prevention of the tibia translating anteriorly to the femur. The counterpart to the ACL, the posterior cruciate ligament (PCL), has similar attachments but is oriented in a way to prevent the tibia from translating posteriorly on the femur.

The use of stem cells to promote healing and regeneration in individuals has been an area of great debate, both casually and in federal and local government. A majority of the debate centers on the use of embryonic stem cells. These types of cells are collecting during an organism’s developing stage and have great implications for their application because the cells are able to differentiate into any other human cell. Research has been limited due to the moral and ethical implications.
Alternatively, adult stem cells hold none of the prior mentioned implications and have shown to be effective in healing many types of tissues. Mesenchymal stem cells, specifically, are the root cell of bone, cartilage, and muscle tendon and are collected from the adult to which the treatment is performed.
In their simplest form, adult stem cells are an undifferentiated cell that can develop into many types of tissue cells. When the stem cell is applied to a certain type of tissue, it will begin to develop into that same tissue and adhere. This type of technique is called “cell therapy” which allows for the stem cell to differentiate while in contact with its intended tissue type. For example, a collection of stem cells are injected in an area where a muscle tendon is injured. The cells begin to adhere to the healthy tissue and form into tendon tissue in place of the injured or absent tissue.
Adult stem cells can be collected from many areas of the body but for the use of orthopedic regenerative medicine two sites are most useful. The first is from bone marrow. Cells are collected from long bone, normally the femur, and concentrated into a solution. Alternatively, and often more comfortable to the patient, stem cells can be collected from adipose tissue. The adipose is then placed in a centrifuge and separated into multiple layers. One of the layers becomes concentrated in stem cells and used during the procedure on the same patient.
The use of adult stem cells has become more common in procedures involving muscles, bones and joints. Because it is a non-surgical procedure and due to lower risk to the individual, these treatments are gaining greater popularity in patients that have failed prior treatments or patients that are looking for an alternative to surgery.
A continuing body of research is developing to support the use of adult stem cell and PRP therapy for orthopedic conditions. In private practice the procedures are being performed in conjunction with other treatment including physical therapy and have shown to be successful. Practitioners that are considering Adult Stem Cell Therapy are advised to seek out the most recent literature and guidelines to assist in their clinic decision-making. Continued examination of the outcomes of the procedure is suggested to identify the best treatment options.
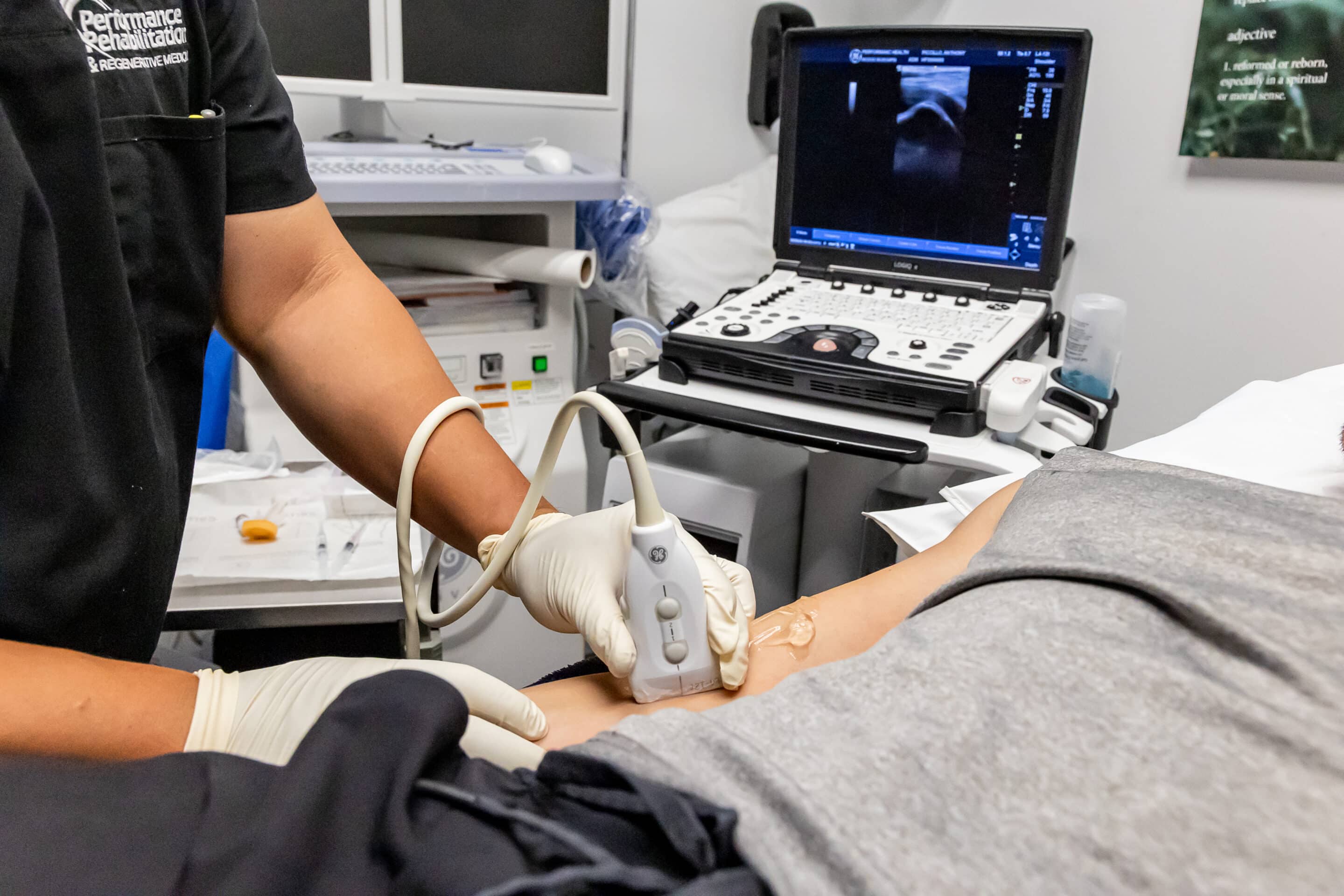
There are many criteria for patients seeking adult stem cell therapy. A comprehensive orthopedic examination is needed as well as other diagnostic tests including MRI, diagnostic ultrasound or x-ray to best determine the pain generator and extent of injury. Anyone interested in these procedures are advised to seek consult from a physician who understands the process and has experience with this treatment. Performance Rehabilitation & Regenerative Medicine is a leader in regenerative medicine and continues to stay at the forefront of the safest and most effective care.
For more information please feel free to contact one of our Patient Care Coordinators today at 908-754-1960 or you may contact us online.
About the Authors:
Joseph Mejia D.O., F.A.A.P.M.& R, is a graduate of University of Michigan and West Virginia School of Osteopathic Medicine. He is Board Certified in Physical Medicine & Rehabilitation and Sports Medicine. Dr. Mejia received his Fellowship Training in Interventional Pain Management from University of Medicine and Dentistry. He has advanced training in Regenerative Medicine and is the Medical Director and Partner of Performance Rehabilitation & Regenerative Medicine.
John F. Ellis, D.C. is a graduate of Logan Chiropractic College. He is a Board Certified Chiropractic Physician with licenses held in New Jersey and New Hampshire. His past research work involves human performance pertaining to orthopedic conditions. Dr. Ellis is a Chiropractic Physician at Performance Rehabilitation & Regenerative Medicine.