Prolotherapy: A promising alternative to traditional orthopedic treatments
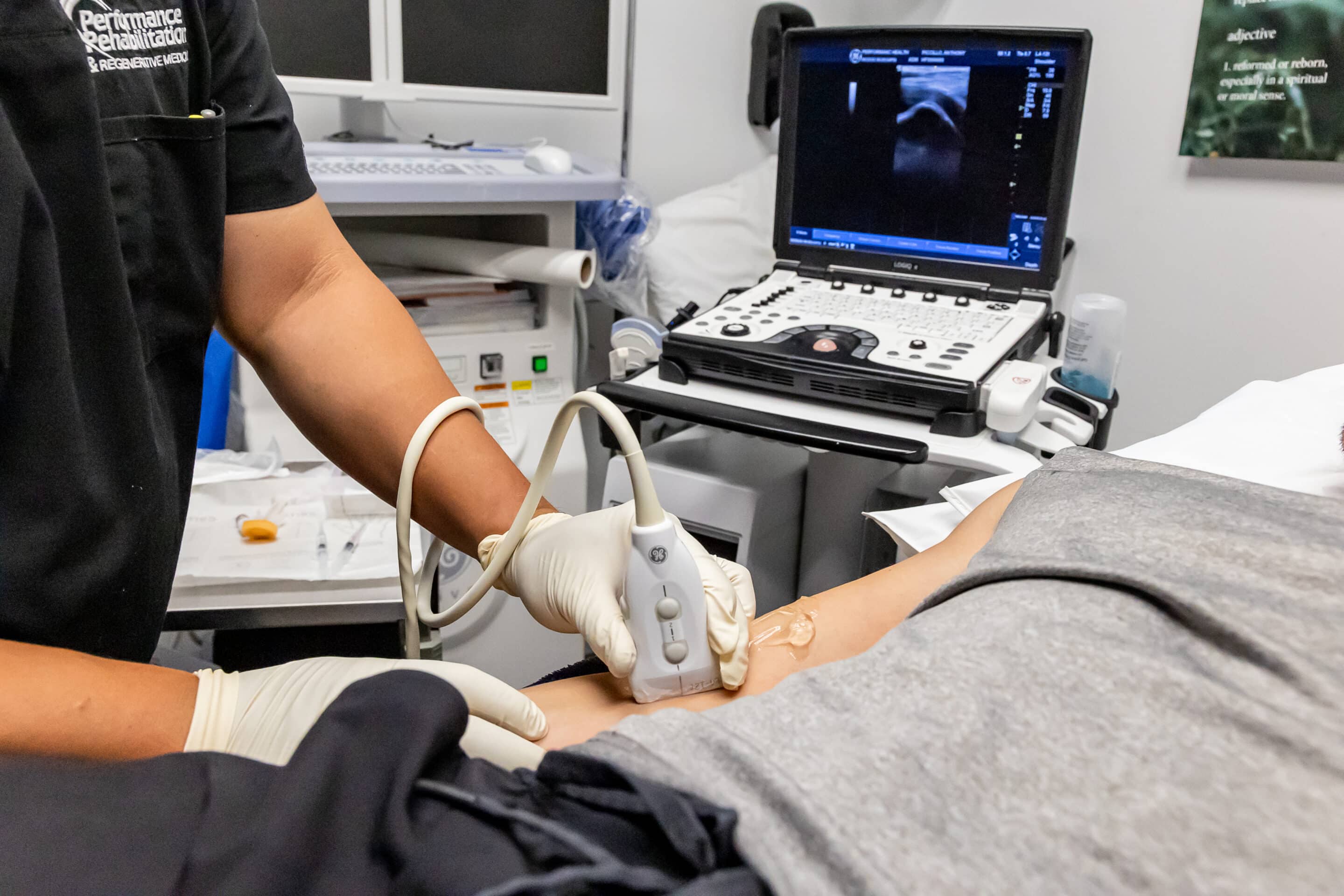
Prolotherapy is a procedure useful for musculoskeletal conditions of a chronic nature, which utilizes injection-based medicine. The procedure involves injecting a small amount of an irritant into painful ligaments and tendons over multiple treatments. The injection of the irritant causes a sequence of events resulting in the activation of fibroblasts leading to an increased strength within the targeted tendon and ligament.4 The most commonly used irritant is a sugar solution containing hyperosmolar dextrose. Other solutions have been used with varying results.
Prolotherapy and Arthritis of the Knee:
Osteoarthritis (OA), often referred to as degenerative arthritis, is a condition commonly affecting the knee. This condition can cause pain, instability and risk of further, more severe knee injuries. As with other degenerative arthritis conditions, osteoarthritis of the knee can be a debilitating ailment often affecting one’s ability to exercise, climb stairs or even walk without difficulty.
Knee OA is understood to be an age-related condition caused by excessive use and stress on the knee joint. Although not exclusive to the older population, knee OA affects 34% of the population over 65 years old.1
Prolotherapy and Injury of the Rotator Cuff:
The rotator cuff is a group of four muscles that produces movement in the shoulder. The four muscles which include the supraspinatus, infraspinatus, teres minor and subscapularis, attach the scapula to the head of the humerus and provide movement and stability to the shoulder. The tendons form a capsule or a cuff around the shoulder joint providing structural support and fun ction movement.
ction movement.
Rotator cuff injury is a common condition of the shoulder that affects individuals from many backgrounds and activities. Injuries of these tendons are understood to impact 1 in 5 adults in their lifetime.2 Common injuries include: tears to the tendon, tendonitis and other tendinopathy.
There are multiple treatment methods that have been utilized to treat rotator cuff injuries and knee OA. More common treatments include pain medication, physical therapy, steroid injection and in some cases surgical intervention.3 Many alternative treatments have been gaining ground in the area of regenerative medicine. One option for treatment is Prolotherapy.
In a long-term outcome study reviewing the efficacy of prolotherapy for knee OA, Rabago et al examined individuals with mild-to-severe OA over the course of 1.5-3.5 years.5 Prior to the study, participants were involved in three separate studies, which examined the effects of prolotherapy over the course of 52 weeks. Rabago et al used the Western Ontario McMaster University Osteoarthritis Index (WOMAC) questionnaire to determine outcomes. This questionnaire evaluates knee OA severity using pain, stiffness and functional subscales.6 Inclusion criteria consisted of knee OA demonstrated on radiograph within five years of initial encounter, tenderness found on one or more anterior knee structures and self-reported pain over at least three months with a score of 3-10 on a 0-10scale
Participants received prolotherapy on at least three separate occasions, at one, five and nine weeks. Optional injections were provided at weeks 13 and 17 based on clinical presentation. Participants in the study were discouraged from using non-steroidal, anti-inflammatory medications (NSAIDs) and from seeking additional care for their knee during the initial follow-up period. This was set in place to ensure more accurate WOMAC scores based on the prolotherapy effects alone.
The average post-treatment follow-up was 2.5 years and showed an improvement in WOMAC scores of 20.9 points, which is 35.6%. 62% of participants improved by at least 12 points and 82% or participants reported some improvement during their long-term follow-up.
In the case of rotator cuff pathologies, the use of prolotherapy was examined in two recent studies. Bertrand, et al compared the use of prolotherapy versus a control saline injection.7 Participants were adults with ages ranging from 19-75 and were seen in a single pain care clinic. Inclusion criteria included pain for at least 3 months, positive orthopedic findings and ultrasound findings of supraspinatus pathologies. Prolotherapy injections were administered at 0, 1 and 3 months intervals into specific tendons and ligaments in the symptomatic shoulder.
Outcome measures included: Ultrasound Shoulder Pathology Rating Scale (USPRS), Visual Analogue Scale (VAS) and numerical rating scale (NRS). Outcomes were measure at 0, 3 and 9 months for VAS and NRS, and within 6-months for the USPRS. Participants were also asked if they believe they received true prolotherapy or were in a sham group.
At the 9-month follow-up, participants that received prolotherapy showed a 2.9-point improvement in pain compared to 1.8 and 1.3 in the control groups. This difference was shown to be somewhat significant. Participant satisfaction at long-term follow-up was shown to be significant among groups with the prolotherapy group showing the highest satisfaction. USPRS scores at a 6-month follow-up showed a slight decrease (improvement) in score but were not shown to be statistically significant.
Lee, at al conducted a retrospective study of prolotherapy on rotator cuff disease at the 1-year follow-up.8 Inclusion criteria included: diagnosis of non-traumatic chronic rotator cuff tendonitis or partial thickness tear, symptoms for more than 3 months, and positive orthopedic exam findings with the correlation between physical exam and radiographic findings.
Outcome measures included VAS score, Shoulder Pain and Disability (SPADI) score, isometric strength of the shoulder abductor, shoulder active range of motion (AROM), maximum tear size on ultrasonography, and number of analgesic ingestions per day. These measures were taken upon initial examination and at 1-year post-injection.
Injections were administered at 0, 2, and 5 weeks. A series of injections continued every 4 weeks until either (1) the level of pain reduced to half of the initial level, (2) patient reached a maximum of 8 rounds of injections, or (3) patient voluntarily withdrew from treatment. The average number of injections was 4.8 over the course of treatment. A control group of similar size and findings was instructed to continue conservative care without prolotherapy. There were no statistical differences in the 2 groups when comparing age, sex, dominant shoulder, and duration is symptoms of ultrasound findings.
In comparing the treatment and control group, the treatment group showed improvements in VAS, SPADI score, isometric strength, and shoulder AROM in flexion, abduction and external rotation. There were no differences seen in the number of analgesic medications taken over the course of care. The most significant outcome was the VAS score of the treatment group compared to the control group over the course of one year.
The use of prolotherapy to treat a variety of orthopedic conditions has a growing body of research to suggest positive patient outcomes in a clinical setting. Practitioners that are considering prolotherapy are advised to seek out the most recent literature and guidelines to assist in their clinic decision-making. Continued examination of the outcomes of the procedure is suggested to identify the best treatment options.
About the Authors:
Joseph Mejia D.O., F.A.A.P.M.& R, is a graduate of University of Michigan and West Virginia School of Osteopathic Medicine. He is Board Certified in Physical Medicine & Rehabilitation and Sports Medicine. Dr. Mejia received his Fellowship Training in Interventional Pain Management from University of Medicine and Dentistry. He has advanced training in Regenerative Medicine and is the Medical Director and Partner of Performance Rehabilitation & Regenerative Medicine.
John F. Ellis, D.C. is a graduate of Logan Chiropractic College. He is a Board Certified Chiropractic Physician with licenses held in New Jersey and New Hampshire. His past research work involves human performance pertaining to orthopedic conditions. Dr. Ellis is a Chiropractic Physician at Performance Rehabilitation & Regenerative Medicine.
References:
- Lawrence RC, Felson DT, Helmick CG, et al. Estimates of the prevalence of arthritis and other rheumatic conditions in the United States. Part II. Arthritis Rheum 2008;58:26—35.
- Yamamoto A, Takagishi K, Osawa T, et al. Prevalence and risk factors of a rotator cuff tear in the general population. J Shoulder Elbow Surg 2010;19:116-20.
- Bishay V, Gallo RA. The evaluation and treatment of rotator cuff pathology. Prim Care 2013;40:889-910. viii.
- Liu YK, Tipton CM, Matthes RD, Bedford TG, Maynard JA, Walmer HC. An in situ study of the influence of a sclerosing solution in rabbit medial collateral ligaments and its junction strength. Connect Tissue Res 1983;11:95-102.
- Rabago D, Mundt M, Zgierska A, Grettie A. Hypertonic dextrose injection (prolotherapy) for knee osteoarthritis: Long term outcomes. Complementary Therapies in Medicine 2015; 23, 388—395 <
- Bellamy N, Buchanan WW, Goldsmith CH, et al. Validation study of WOMAC: a health status instrument for measuring clinically important patient relevant outcomes in antirheumatic drug therapy in patients with osteoarthritis of the knee. J Rheumatol 1988;15:1833—40.
- Bertrand H, Reeves KD, Bennett CJ, Bicknell S, Cheng A. Dextrose Prolotherapy Versus Control Injections in Painful Rotator Cuff Tendinopathy. Archives of Physical Medicine and Rehabilitation 2015;003-993. < .>
- Lee D, Kwack K, Rah UW, Yoon S. Prolotherapy for Refractory Rotator Cuff Disease: Retrospective Case-Control Study of 1-Year Follow-Up. Archives of Physical Medicine and Rehabilitation 2015;96:2027-32. < >