Using science to enhance the body’s natural healing abilities to treat athletic injuries, with Regenerative Medicine
Athletes are always seeking conservative, drug-free treatment options to help them achieve an improved state of health and performance while avoiding unnecessary surgery or medication. One of the fastest-growing sectors of non–surgical orthopedic treatment is the exciting new specialty of Regenerative Medicine, which is more descriptively referred to as “ortho-biologics.” When separated into two terms: the first, “ortho” for orthopedic medicine and the second “biologics”, which means using a substance derived from human sources (usually stem cells or platelets) to treat diseased or dysfunctional soft tissue. Soft tissue includes muscles, ligaments, tendons and cartilage.
The two most common types of Regenerative Medicine procedures that are helping athletes avoid invasive orthopedic surgery are Platelet Rich Plasma Therapy (PRP) and Adult Stem Cell Therapy.
In clinical practice, it can be very frustrating for the patient and clinician when confronted with soft tissue injuries that are not responding as quickly as we would expect. One of the limiting factors for soft tissue to heal and repair is that the structures are relatively avascular. A limited blood supply will often result in incomplete healing and resultant scar tissue formation. Platelet Rich Plasma Therapy is a promising treatment for soft tissue injuries by increasing the vascular content to the injured site.
NJ Regenerative Medicine – Platelet-Rich Plasma and Adult Stem Cell Therapy
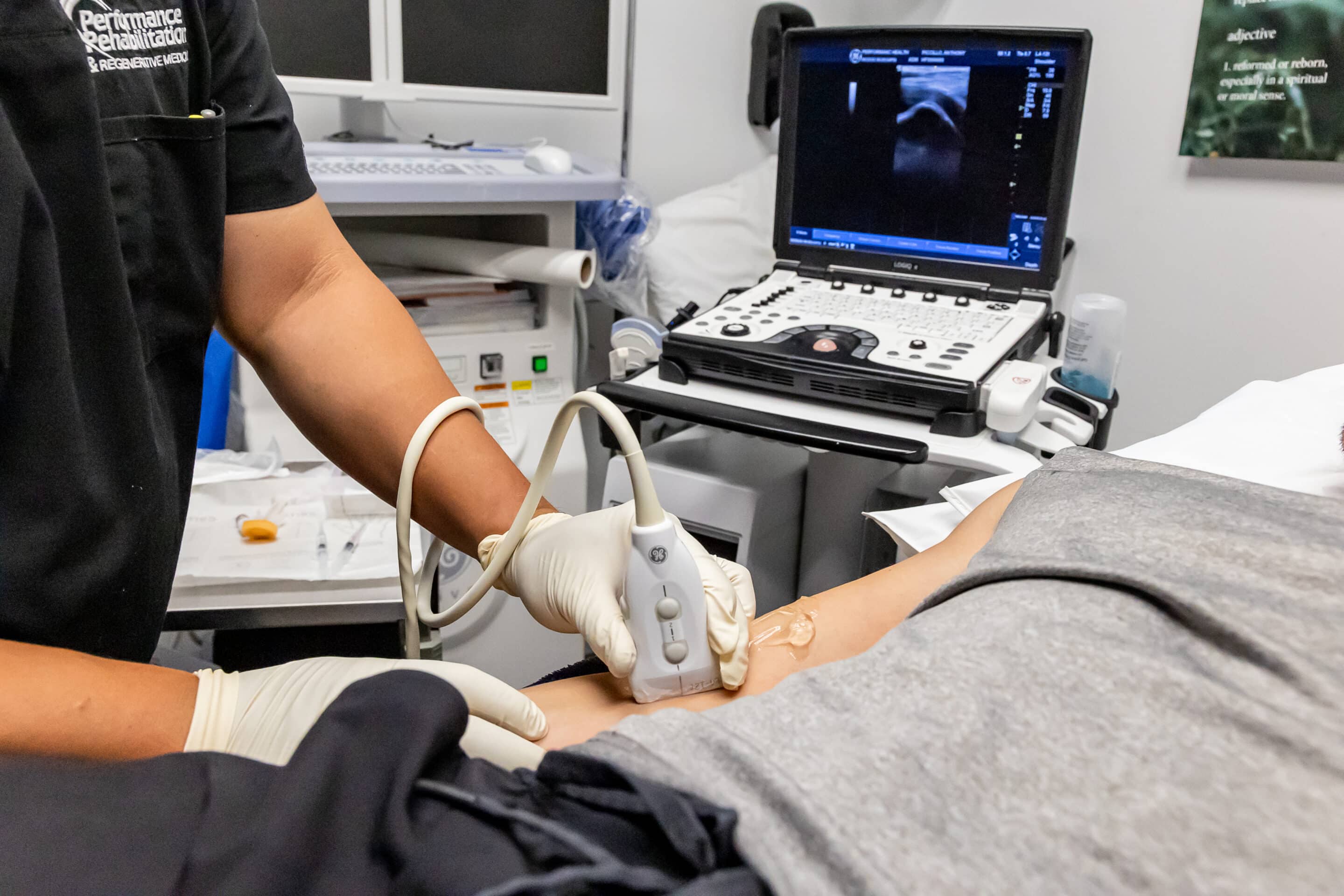
The basic princi ples of PRP are quite simple. Platelets are small, non-nucleated cells found in human blood, which are essential for healing. In a typical PRP application, blood is drawn from the patient and processed in a centrifuge to separate blood plasma from the natural concentration of platelets, creating a platelet graft matrix. After the PRP graft is obtained, it is then reintroduced into the specific site of injury, via ultrasound-guided imaging. The growth factors, cytokines and adhesion proteins found in the newly grafted PRP matrix activate the necessary stages of tissue healing. The most recent research demonstrates that a PRP graft contains 500 to 600 percent more healing proteins then would naturally occur in injured human tissue. This enhances the patient’s natural ability to recover from injury and reduces healing times.
ples of PRP are quite simple. Platelets are small, non-nucleated cells found in human blood, which are essential for healing. In a typical PRP application, blood is drawn from the patient and processed in a centrifuge to separate blood plasma from the natural concentration of platelets, creating a platelet graft matrix. After the PRP graft is obtained, it is then reintroduced into the specific site of injury, via ultrasound-guided imaging. The growth factors, cytokines and adhesion proteins found in the newly grafted PRP matrix activate the necessary stages of tissue healing. The most recent research demonstrates that a PRP graft contains 500 to 600 percent more healing proteins then would naturally occur in injured human tissue. This enhances the patient’s natural ability to recover from injury and reduces healing times.
Adult stem cell therapy is at the forefront of Regenerative Medicine, which many believe is changing the field of orthopedic medicine. Adult stem cells should not be confused with the controversial embryonic stem cells, as the adult stem cells are obtained directly from the patient. Stem cells are undifferentiated cells, which have the ability to be “turned on” into any cell type to repair and regenerate injured tissue. We are seeing tremendous results with healing partial tendon and ligament tears, that were previously unresponsive to treatment.
Due to recent improvements in modern medicine, stem cells (adult) can now be obtained through a simple medical harvesting procedure directly from the patient in a painless process done in the office. Once the physician obtains the stem cells they are immediately processed in the office to create a healing matrix of stem cells.
Similar to PRP, the stem cell matrix is then grafted onto the injured site aide by advanced computer-guided ultrasound imaging and MRI evaluation. It is advised that the region, which has received the stem cell graft, be rested and immobilized for several days to ensure the graft doesn’t dislodge. Patients must realize this is not a “quick fix”, as it a reparative process that can take up to 2-3 months.
Sometimes stem cell therapy and PRP therapy are performed on the same injury. The physician will make this determination after reviewing all diagnostic information.
The injections are extremely safe and the risk is minimal as it is “body to body” transmission, thus eliminating the risk of disease transmission or of the body rejecting the graft. The only side effect we have seen over the past 4 years is soreness at the injection site after the procedure.
In our office, the conditions with which we have seen the greatest success include:
- Chronic tendonitis, such as tennis or golfer’s elbow
- Rotator cuff tendonitis
- Plantar fasciitis
- Achilles tendonitis
- Wrist tendonitis (De Quervain’s syndrome)
- Patellar tendonitis
We have also successfully treated glenoid labral tears, as well as moderate osteoarthritis of the shoulder, knee and hip.
If you have any questions about Regenerative Medicine or would like to make an appointment with one of our physicians, please contact our Patient Care Department at 908-756-2424 or you may contact us online.
About the author:
Joseph Mejia D.O., F.A.A.P.M.&R, Is a graduate of University of Michigan and West Virginia School of Osteopathic Medicine. He is Board Certified in Physical Medicine & Rehabilitation and Sports Medicine. Dr. Mejia received his Fellowship Training in Interventional Pain Management from University of Medicine and Dentistry. He is the Medical Director and practice Partner of Performance Rehabilitation & Regenerative Medicine.